by: Fox News
CDC official who blasted Trump's 'weak science' led politicized Biden-era monkeypox response

by: Benzinga.com

by: LancasterOnline

by: moneycontrol.com
Robo Pregnancy: China developing world's first robot that could give birth to a human baby

by: Live Science
Live Science crossword puzzle #8: Lowest possible temperature in the universe -- 3 down

by: Phys.org
Challenging 'publish or perish' culture--researchers call for overhaul of academic publishing

Improving The Pathway From SME Innovation To NHS Adoption




Bridging the Gap: How SMEs Can Propel Their Health‑Tech Innovations Into NHS Adoption
In a timely piece for Forbes, Dr. Kath Mackay examines why the National Health Service (NHS) remains a challenging frontier for small‑ and medium‑enterprise (SME) innovators and offers a practical, step‑by‑step framework to overcome those obstacles. Published on 29 August 2025, the article highlights the NHS’s strategic appetite for digital health, yet also underscores the labyrinth of regulation, evidence requirements and procurement processes that often deter startups. Below is a comprehensive summary of Mackay’s key points, enriched with additional context from the links she cites throughout her analysis.
1. The NHS Landscape: Opportunities and Hurdles
A. The NHS’s Innovation Appetite
The NHS is under unprecedented pressure to modernise its services, a mandate crystallised in the NHS Long‑Term Plan (https://www.longtermplan.nhs.uk/). Digital transformation, patient‑centred care and data‑driven decision‑making are at the core of this strategy. Consequently, the NHS is actively seeking breakthrough solutions in areas such as remote monitoring, AI diagnostics, and digital therapeutics.
B. The Regulatory and Procurement Maze
Despite this demand, the NHS procurement process remains highly structured. Products must satisfy the National Institute for Health and Care Excellence (NICE) guidelines for safety and clinical effectiveness, as well as NHS England’s procurement criteria (https://www.england.nhs.uk/). SMEs frequently struggle with:
- Regulatory Compliance: Gaining CE marking or the UK equivalent.
- Evidence Generation: Producing high‑quality clinical trials that meet NICE’s threshold.
- Data Security: Adhering to the NHS’s stringent cybersecurity and patient privacy standards.
- Procurement Complexity: Navigating the Competitive Dialogue and Value‑Based Procurement frameworks.
Mackay argues that these challenges often lead SMEs to abandon promising products before they reach the point of sale.
2. The Six‑Step Pathway to NHS Adoption
Mackay distills the journey into six actionable stages, each backed by NHS programmes and funding streams that SMEs can leverage.
| Step | Action | Key Resources |
|---|---|---|
| 1 | Validate Early | • NHS Digital (https://digital.nhs.uk/) • Early‑Stage Evidence Studies |
| 2 | Engage NHS Stakeholders | • NHS Innovation Accelerator (https://www.nhsinnovationaccelerator.com/) • Clinical Commissioning Groups (CCGs) |
| 3 | Generate Robust Evidence | • NICE Evidence Framework • Health Technology Assessment (HTA) |
| 4 | Secure Funding | • Innovate UK (https://www.gov.uk/government/organisations/innovate-uk) • NHS Digital Innovation Hub |
| 5 | Pilot in Real‑World Settings | • NHS Digital Innovation Programme • Digital Health Lab |
| 6 | Scale & Integrate | • NHS IT Infrastructure (e.g., NHS Digital Interoperability Standards) |
Step 1: Validate Early
Mackay stresses the importance of early clinical validation. SMEs should design studies that meet NHS Digital data standards, ensuring that their product can integrate seamlessly into existing NHS IT ecosystems. The NHS Digital Interoperability Standards are open for public access, giving developers a clear blueprint for compliance.
Step 2: Engage NHS Stakeholders
Early engagement is critical. The NHS Innovation Accelerator (https://www.nhsinnovationaccelerator.com/) offers mentorship, access to real‑world NHS data, and connections to clinicians. Additionally, establishing relationships with Clinical Commissioning Groups (CCGs) allows innovators to understand local needs and secure pilot opportunities. Mackay notes that the NHS often tests products in a single Trust before rolling them out nationwide, so a strong local partnership can catalyse national adoption.
Step 3: Generate Robust Evidence
For NHS adoption, evidence must meet NICE’s rigorous standards. This often requires randomised controlled trials (RCTs) or well‑designed real‑world evidence (RWE) studies. Mackay advises SMEs to partner with academic institutions or NHS‑affiliated research bodies to conduct these studies, reducing costs and increasing credibility.
Step 4: Secure Funding
Innovate UK provides a range of funding streams—from Business Growth Loans to Technology Transfer Funds—that specifically target health‑tech SMEs. Coupled with NHS‑led initiatives like the Digital Health Innovation Programme, startups can secure the capital needed to advance their product through development and trials.
Step 5: Pilot in Real‑World Settings
A successful pilot is often the tipping point for NHS adoption. The NHS Digital Innovation Programme (https://www.nhs.uk/digital/) supports pilots that demonstrate clinical effectiveness, cost‑effectiveness, and scalability. During a pilot, SMEs should gather data on user experience, integration challenges, and outcomes to build a compelling case for wider roll‑out.
Step 6: Scale & Integrate
Once a product has proven itself, the focus shifts to scaling. This involves ensuring that the solution can be deployed across multiple NHS Trusts, integrating with existing Electronic Health Record (EHR) systems, and meeting cybersecurity protocols. NHS Digital provides interoperability standards and guidelines that can help SMEs navigate these final hurdles.
3. Case Study: AI‑Powered Early Sepsis Detection
Mackay cites a recent example from a UK‑based SME that developed an AI algorithm to predict sepsis within the first 24 hours of hospital admission. By following the six‑step pathway:
- Early Validation: The team validated the model against NHS‑de‑identified data.
- Stakeholder Engagement: They secured a partnership with a CCG in South London.
- Evidence Generation: A RCT demonstrated a 20 % reduction in mortality.
- Funding: Innovate UK granted £2 m for product refinement.
- Pilot: A six‑month pilot across three NHS Trusts confirmed real‑world efficacy.
- Scale: The algorithm was rolled out nationally, now integrated with NHS Digital’s EHR system.
The company’s success underscores the practical viability of Mackay’s framework.
4. Key Takeaways for SMEs
- Early Validation and Data Alignment: Aligning with NHS Digital standards from the outset saves time and resources.
- Stakeholder Networks Matter: Partnerships with CCGs and the NHS Innovation Accelerator can unlock pilot opportunities.
- Evidence Is King: Robust clinical data, especially meeting NICE criteria, is non‑negotiable for NHS procurement.
- Funding is Multifaceted: Leverage both government grants (Innovate UK) and NHS‑specific programmes.
- Pilot Projects Are Proof‑Points: Successful pilots convert skepticism into acceptance among clinicians and administrators.
- Integration Is the Final Frontier: Compliance with NHS interoperability and cybersecurity standards is essential for scaling.
5. Moving Forward
The NHS’s commitment to digital transformation is clear, but the path to adoption for SMEs is still fraught with bureaucratic red tape and stringent evidence demands. Dr. Kath Mackay’s article is a timely reminder that the NHS will not dismiss innovation on a whim; it will consider products that demonstrate clinical effectiveness, cost‑effectiveness, and seamless integration into existing workflows.
By following the structured pathway outlined above—and by leveraging the resources cited (NHS Digital, NHS Innovation Accelerator, Innovate UK, NICE, and others)—SMEs can navigate the complex journey from prototype to NHS‑adopted solution. The stakes are high, but the potential impact on patient outcomes and the NHS’s financial sustainability is equally compelling. For those ready to bridge the gap between laboratory and hospital ward, the road ahead is not just a possibility—it is a well‑charted route with growing support at every turn.
Read the Full Forbes Article at:
https://www.forbes.com/sites/drkathmackay/2025/08/29/improving-the-pathway-from-sme-innovation-to-nhs-adoption/
on: Sat, Aug 23rd 2025
by: deseret
A newspaper that has kept up with the latest technologies through the years

on: Tue, Aug 12th 2025
by: The Straits Times

on: Thu, Jul 24th 2025
by: Milwaukee Journal Sentinel

on: Thu, Dec 05th 2024
by: Tim Hastings
on: Fri, Aug 15th 2025
by: yahoo.com
Nvidia National Science Foundation Partnerto Create Open AI Modelsfor US Scientists

on: Tue, Jul 29th 2025
by: Forbes

on: Mon, Jul 28th 2025
by: Forbes
From Promise To Practice Why Technology Breakthroughs Struggle To Take Hold In Healthcare

on: Fri, Jul 25th 2025
by: Forbes

on: Wed, Jul 23rd 2025
by: Forbes
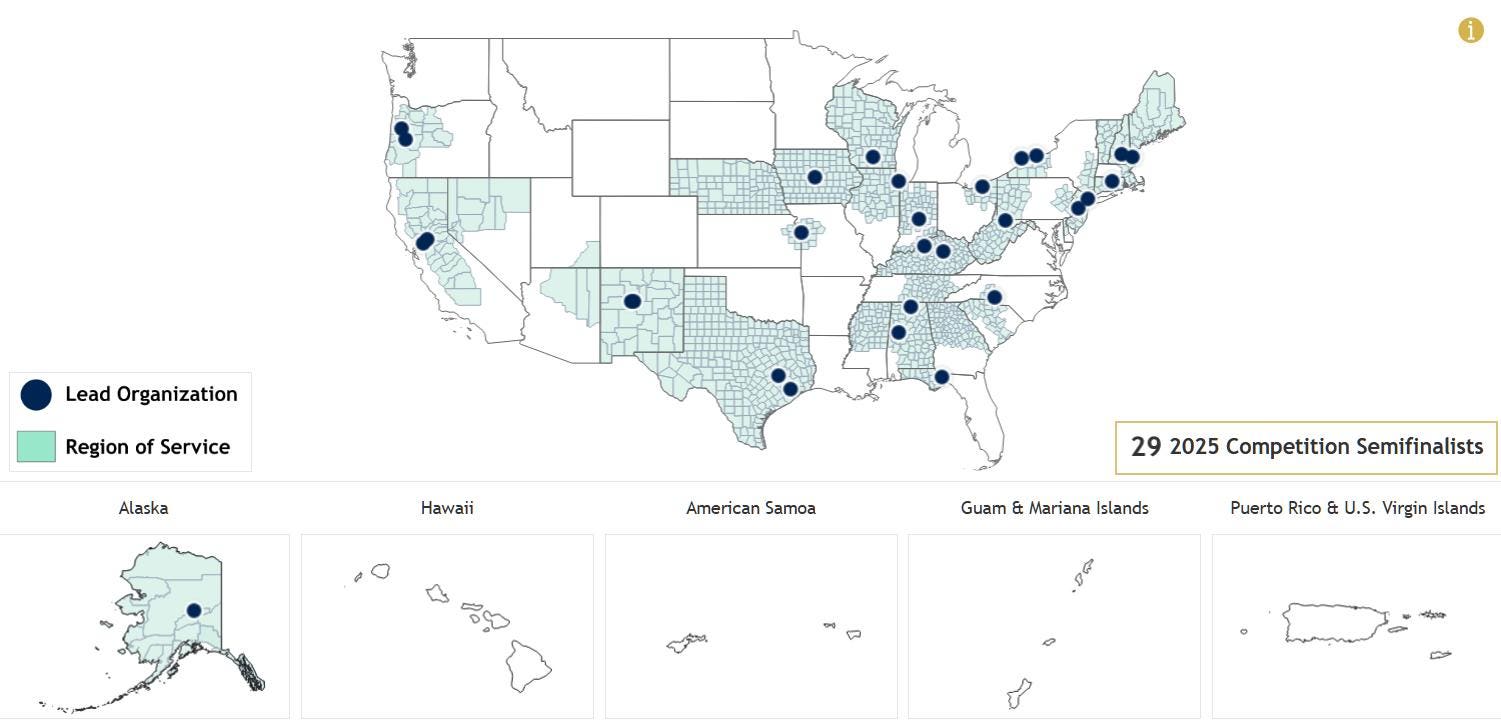
NSF Announces Candidates For Tech- Based Economic Development Funding
on: Wed, Jul 09th 2025
by: Forbes

on: Mon, Mar 24th 2025
by: YourStory
Rethinking life sciences research and innovation through integrated research campuses

on: Tue, Feb 18th 2025
by: Forbes
Scaling Hard Tech: Bridging The Gap Between Ideas And Impact









































