AI Patient Burnout: A Growing Threat to Digital Health





Tuesday, March 10th, 2026 - The promise of digital health - readily available data empowering individuals to take control of their wellbeing - is facing a growing, and potentially debilitating, challenge: 'AI patient burnout.' This phenomenon, explored in depth during a recent Newsweek-hosted webinar, suggests that the relentless stream of health data and notifications generated by wearable technology and virtual care platforms is overwhelming users, leading to disengagement and potentially harming the very health outcomes these tools are designed to improve.
The concept, relatively new to mainstream healthcare discourse, describes a state of exhaustion and apathy arising from constant monitoring and data delivery. While individuals initially embrace these technologies for their proactive approach to health, the sheer volume of information can quickly become paralyzing. It's a paradoxical situation: tools meant to empower are instead causing users to tune out.
"It's not that the technology isn't useful, but we're creating situations where patients are receiving too much information," explained Dr. Michael Malone, Chief Medical Officer at Access Health, during the webinar. "We're essentially drowning them in data, and they're shutting down." This 'drowning in data' isn't simply about the quantity, but also the lack of meaningful interpretation. Raw data points - heart rate variability, sleep stages, activity levels, blood glucose readings - without contextualization or actionable insights, are largely useless and contribute to the feeling of being overwhelmed.
The problem extends beyond simple annoyance. Dr. Lena Hanson, a behavioral psychologist specializing in health technology adoption, who wasn't on the original panel but has extensively researched this area, notes that chronic exposure to overwhelming stimuli can trigger a stress response. "The constant notifications, the pressure to 'optimize' health metrics, can create a feedback loop of anxiety," she explains. "People begin to associate self-monitoring with negative emotions, leading them to abandon the tools altogether."
Companies like Oura, renowned for its popular sleep and activity tracking ring, and Access Health, a leading virtual primary care provider, are acutely aware of this potential pitfall. Both organizations were represented on the panel, highlighting their commitment to user-centered design. Ashley Thompson, Head of Health Partnerships at Oura, emphasized the crucial role of human connection. "The conversation has to be human," she asserted. "We need to be careful about how we're communicating with patients. AI should be a tool to help doctors and patients, not a replacement for that relationship."
This sentiment underscores a growing concern that the focus on technological advancement may be overshadowing the importance of the patient-physician relationship. The ideal scenario, panelists agreed, isn't a fully automated system, but a hybrid model where AI assists healthcare professionals in providing more personalized and effective care. AI can handle data analysis and identify potential issues, but the crucial interpretation and communication should remain with a human provider.
So, what solutions are being proposed? Prioritization and contextualization are key. Rather than simply presenting a barrage of raw data, AI algorithms need to be refined to deliver insights tailored to each individual's needs, goals, and lifestyle. For example, instead of just displaying a sleep score, the AI could identify specific patterns affecting sleep quality and offer personalized recommendations for improvement. Similarly, activity data could be framed in relation to the patient's fitness level and long-term health objectives.
Furthermore, the industry is beginning to address the ethical considerations surrounding AI in healthcare. Data privacy remains a paramount concern, and ensuring algorithmic fairness is crucial to avoid exacerbating existing health disparities. Transparency - allowing users to understand how the AI is making recommendations - is also vital for building trust and fostering engagement.
The webinar also raised questions about the responsibility of developers and healthcare providers to educate patients about the appropriate use of these technologies. Many users may not fully understand the limitations of wearable sensors or the potential for inaccurate data. Clear and concise explanations, coupled with realistic expectations, are essential for preventing frustration and ensuring that patients can benefit from these tools without experiencing burnout.
The issue of 'AI patient burnout' isn't a technological problem, but a design and implementation problem. It's a stark reminder that technology, no matter how advanced, must always be centered around the needs and wellbeing of the individual. The future of digital health hinges on striking a delicate balance between data-driven insights and human-centered care.
Read the Full Newsweek Article at:
https://www.newsweek.com/ai-patient-burnout-webinar-oura-access-health-11637599
on: Thu, Mar 05th
by: reuters.com

on: Fri, Feb 20th
by: whitehouse.gov

on: Thu, Feb 19th
by: KXAN
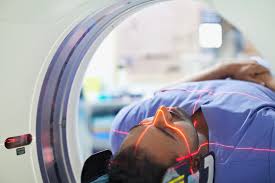
AI-Powered CT Scan Revolutionizes Patient Care at Austin Hospital
on: Mon, Feb 16th
by: Business Today

on: Mon, Jan 26th
by: The Baltimore Sun

on: Sun, Feb 15th
by: RepublicWorld

on: Sun, Feb 15th
by: moneycontrol.com

on: Thu, Feb 12th
by: Newsweek

on: Sun, Feb 01st
by: Dallas Morning News

on: Sun, Jan 18th
by: Seeking Alpha
BlackRock Science & Technology Trust: AI Investment Opportunity

on: Fri, Jan 09th
by: deseret

on: Wed, Nov 05th 2025
by: Forbes
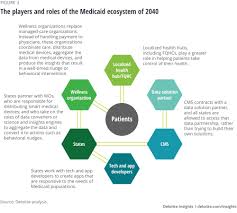
The Role Of Technology And Innovation In The Future Of Medicaid